
Richard G. “Bugs” Stevens, University of Connecticut
Does glyphosate, the active ingredient in the widely used weedkiller Roundup, cause non-Hodgkin lymphoma? This question is at issue now in a lawsuit in San Francisco Superior Court. Hundreds more claims have been cleared to proceed in a federal multi-district lawsuit.
Much of this litigation is based on a 2015 determination by the International Agency for Research on Cancer, part of the World Health Organization, that glyphosate is a probable human carcinogen. This report has come under heavy criticism, which is not surprising because there’s a lot of money at stake.
The IARC classification relied in part on experiments in mice. But is that enough to conclude the weed killer causes cancer in humans? Mice are not people, so probably not.
If it was simple to determine the cause of cancer in humans, scientists would do the right experiment and we’d know the answer pretty quickly.
But it’s not simple.
Proving causation in product liability lawsuits
Epidemiology is one of the sciences that provides evidence needed to prove cause and effect in medicine and public health. It is the most important tool for determining whether exposure to a given substance increases the risk of disease. The problem is that it is easy to do it badly, and a bad study is worse than no study at all.
In fact, after a special hearing examining the science on both sides of the glyphosate argument, U.S. District Judge Vince Chhabria called epidemiology “loosey-goosey” and a “highly subjective field.” Nonetheless, he concluded that the views on both sides were reasonable and should be heard in court, with the verdict up to a jury.

AP Photo/Seth Perlman
I have spent much of my working life trying to help figure out why people get cancer. To illustrate how hard it is to prove causality, consider the question: Does smoking cause lung cancer?
Innumerable epidemiological studies since the 1940s have shown a strong association between smoking and lung cancer. But there has never been a randomized trial in humans. In addition, we know from experimental studies that smoking rats don’t get lung cancer.
For years, Big Tobacco dismissed observational studies in people (epidemiology) with the mantra that “association is not causation,” and avoided regulation. The scientific community was intimidated by this strategy for far too long. Eventually, the studies accumulated to the point that the association was overwhelming, and cause and effect could not be denied.
There are two main types of epidemiological study designs: cohort and case-control. In a cohort study, a large group of people – some smokers, some not – are followed over the years to see who gets sick. In a case-control study, a group of lung cancer patients (perhaps several hundred) are asked about their smoking history, along with an equal number of people without lung cancer.
Invariably, in cohort study after cohort study, smokers got sicker from heart disease, lung cancer and many other maladies over time. In most of these studies, scientists did their best to take account of other differences between smokers and non-smokers, so as to isolate the effect of smoking. Also invariably, in case-control studies patients with lung cancer were much more likely to have been smokers than people in the general population.
Defining ‘proof’
When scientists are asked for a definition of proof, most of them use criteria such as “reproducibility” and “statistical significance” and “plausibility.” But who decides whether each of these criteria has been met? The answer is a panel of experts. It is unsettling to most scientists to hear that “proof” can only be defined as “a consensus of experts,” but this is true from physics to bird-watching. And what has been proven can later be unproven with new experts and/or new evidence.
Who chooses the experts? They include panels convened by the National Academies of Sciences, or advisory boards of professional societies such as the American College of Cardiology. The makeup of these panels can be challenged, and of course, people can choose to ignore the “experts” and believe what they want.
In health research, “causing” disease is defined as “increasing risk.” This does not mean that exposure to something like cigarettes is both necessary and sufficient to cause disease. Most heavy smokers never get lung cancer, and some lifelong non-smokers do. However, experts agree that smoking causes lung cancer because hundreds of observational epidemiological studies show that a heavy smoker has a risk of lung cancer 10 to 20 times higher than a non-smoker. This agreement among experts is the proof that smoking causes lung cancer.

AP Photo/hwg
For many other potential hazards, the epidemiology is either inadequate or contradictory. One study may show an association between exposure and disease, while another shows no relationship. This can happen because the exposure does not cause the disease, and studies that do show a relationship are due to chance, bias and/or confounding – in other words, they are false positive results. It also can happen because the true exposure has not been accurately measured, so existing research is masking a real causative effect – also known as a false negative result.
The process of proving cause in science is quite similar to a jury trial. Evidence is presented to a jury (the expert panel or committee), which renders a verdict. To a “reasonable” person, does the evidence rise to the level of guilt – or, in science, proof of cause and effect?
A health scientist sees proof of causation when evidence from epidemiology (observational studies in people) and toxicology (experiments in rats), and, to some extent basic science (does a chemical damage DNA in a test tube?) accumulates to the point where there is no other viable explanation for the evidence than cause and effect. Epidemiology is paramount, because it is a direct assessment of risk in human beings. It is analogous to circumstantial evidence in a jury trial.
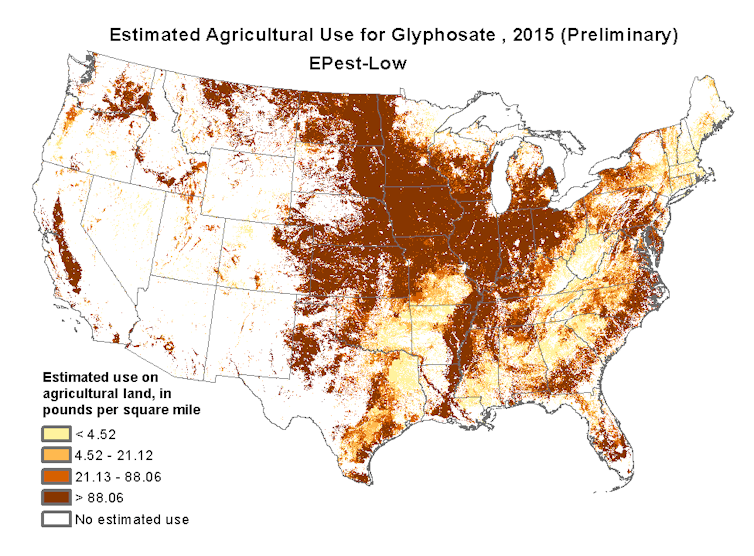
USGS
Is circumstantial evidence enough?
The fact that smoking causes lung cancer is accepted beyond a reasonable doubt based on the circumstantial evidence of numerous observational epidemiological studies. A convincing case for guilt can rest entirely on circumstantial evidence when that evidence is extensive and strong enough to convince a panel of experts.
It will be harder for jurors in the Roundup trials to weigh epidemiological evidence that glyphosate caused plaintiffs’ cancer, because jurors are rarely experts and successful trial lawyers are exceptionally persuasive.
In my view, there are two crucial requirements for an equitable assessment of proof of causation from products like glyphosate or cigarettes. First, were the epidemiological studies well done? Second, how objective are the jurors and the expert witnesses?
Both science and the judicial system are highly imperfect. The verdicts in these trials could be wrong, and could be appealed. This happens as often in the worlds of science and medicine as it does in the courtroom.
![]() It took many years to develop a broad consensus on cigarettes. Unfortunately for the plaintiffs in the Roundup litigation, the same may be true for glyphosate.
It took many years to develop a broad consensus on cigarettes. Unfortunately for the plaintiffs in the Roundup litigation, the same may be true for glyphosate.
Richard G. “Bugs” Stevens, Professor, School of Medicine, University of Connecticut
This article was originally published on The Conversation. Read the original article.




















