By Graham Cookson, University of Surrey
Running a healthcare system is expensive. At present we spend about 8% of our Gross Domestic Product (GDP) on the NHS. The UK’s Office for Budget Responsibility, predicts that by 2061 we could be spending as much as 17% of GDP on healthcare – or roughly half of every pound raised in government revenue.
NHS England chief executive Simon Stevens has set out a blueprint for further investment in the NHS in the NHS Five-Year Forward View. It’s an ambitious plan that would see funding redirected from hospitals into the community and GP surgeries – where procedures such as minor surgeries or scans would be carried out – and greater integration between primary and secondary care. It would reduce demand for care through radical changes to public health – tackling smoking, alcohol misuse and obesity head on – including more input from employers in the form of cash incentives.
To do this, the NHS needs an additional £8 billion over the next parliament (over the existing real-term budget increases) to overhaul the health service. According to Stevens, the money is needed to “lubricate these changes.” The argument is that by spending £8 billion now, the £30 billion funding gap the NHS has can be plugged. Crudely put, if this were to be paid out of general taxation it would amount to roughly an additional £300 per household in tax.
A question of productivity
The plan, however, is big on vision and low on detail. How exactly would that £8 billion be spent and how, and more importantly, when will we see a return on this investment?
What we’re really interested in here is productivity growth. To fill the funding gap, the NHS needs to grow productivity by 3-5%. It’s currently growing (at best) by less than 1% and is quite likely flat. But at the heart of the Five-Year Forward proposal is the promise that productivity can increase from an 0.8% improvement each year to a staggering 3% (the King’s Fund has previously proposed 4% elsewhere). Without any evidence to the contrary this appears to be pure fantasy. For example, over the decade to 2007, private sector productivity grew by 2.3% per year.
Productivity is the amount of healthcare produced for the amount of resources or inputs used. Treating more patients, better for the same or fewer resources would result in rising productivity. Yet the NHS’ record on productivity improvement is poor. Over the decade to 2010 it fell by 0.2% per annum. There are also few signs that the 5% productivity gains required to meet the Nicholson Challenge – the requirement to find £20 billion in efficiency savings – have been met.
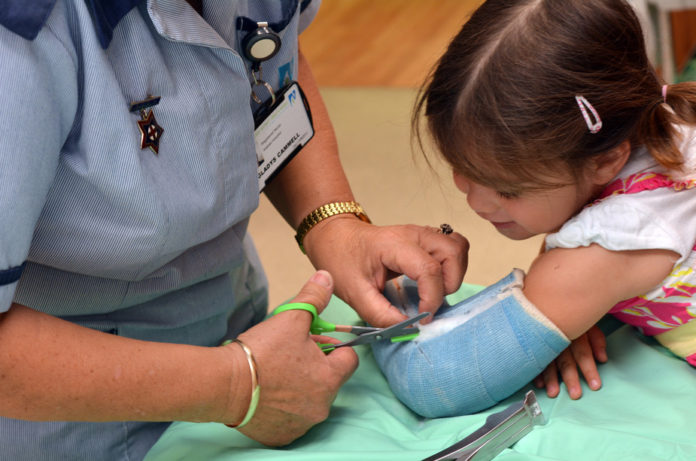
The fundamental problem is that healthcare is delivered by people; it’s a service sector. And as such it suffers from the infamous Baumol cost disease problem. Originally applied to performers, the argument goes that it takes exactly the same number of people to play one of Beethoven’s string quartets as it did in the 19th century. Their productivity hasn’t risen yet their wages have. Similarly, it takes the same amount of time to bandage a wound today as it did 50 years ago.
While this illustration is an oversimplification, it is true that in labour-intensive fields such as healthcare it is difficult to make large improvements in productivity that outstrip rises in the real wage rate. Baumol’s problem is an incurable disease, and one which this latest proposal fails to address head on.
Tied to this is the specific issue of wages in the NHS. The failure of the government to honour the Pay Review Body’s suggested 1% pay rise to NHS staff sparked a wave of industrial action. Trades unions argue that NHS employees have suffered a 15% real wage cut since the last election. To retain high-quality staff and to keep sickness and turnover rates low, the NHS will need to increase wages, especially if there are signs of a strong economic recovery or high private sector wage growth.
Wages represent roughly 55% of NHS expenditure and in the wake of the Francis Inquiry following the Mid-Staffordshire Trust scandal, staffing levels are growing – by almost 2% in the past year.
Bold visions for the NHS should be welcomed. However, before government and the public back further investment it would be wise to understand exactly how this £8 billion would be invested. Perhaps I’m sceptical, but at present there is little evidence to support the claim that such significant growth in NHS productivity is even possible, let alone likely.
![]()
Graham Cookson currently receives funding from The Leverhulme Trust, The National Institute for Health Research, The National Institute for Health and Care Excellence, The Department for Health, The Bar Council, and The Baring Foundation. In addition, he has previously received funding from The Economic & Social Research Council, Centre for Workforce Intelligence, The Law Society of England & Wales, The Metropolitan Police Federation, Spire Healthcare Limited. He is affiliated with The London Borough of Southwark as a Local Education Authority governor for Highshore School. He is a fellow of the Royal Statistical Society and a member of the Royal Economic Society.
This article was originally published on The Conversation.
Read the original article.